Vascular and Periorbital Effects
In selected indications such as dark circles, the visible improvement may involve more than simple
camouflage. Better support of the local tissue environment may influence the appearance of vascular
show-through, shadowing and periorbital depression.
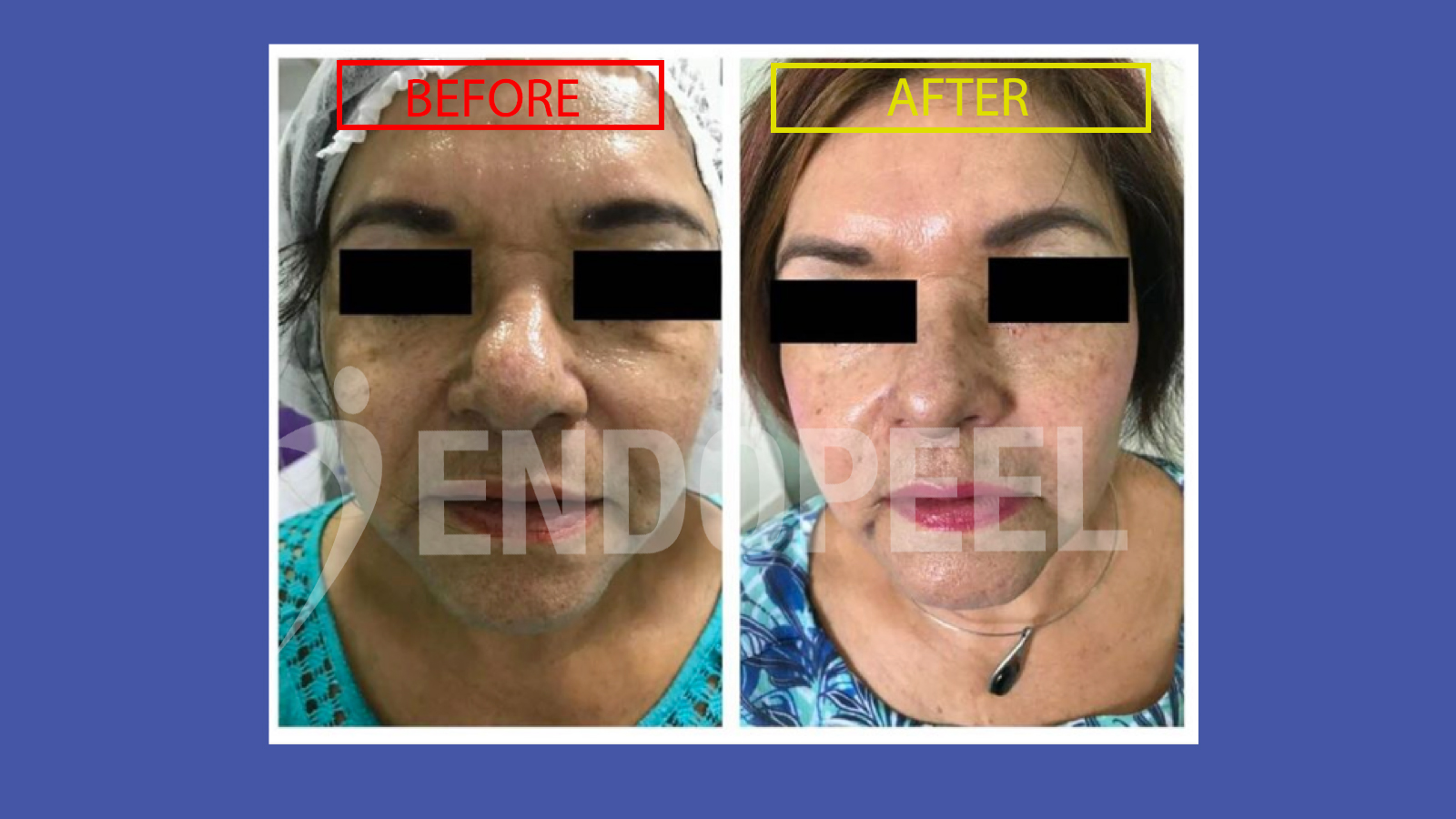
Periorbital dark circles are known to have a multifactorial origin including vascular
show-through, tear trough depression, shadowing effects and, in some cases,
pigmentary components. Structural support of the periorbital tissue may therefore
modify the optical appearance of the region by reducing shadowing and improving
light reflection across the lower eyelid contour.
The effect on vessels should therefore be interpreted cautiously and in context: not as a classic vascular
treatment, but as a structural intervention that can modify how the overlying tissues behave and how
vascular coloration becomes clinically visible.
Periorbital implication:
improvement may result from better support, reduced transparency effect and modified light reflection.